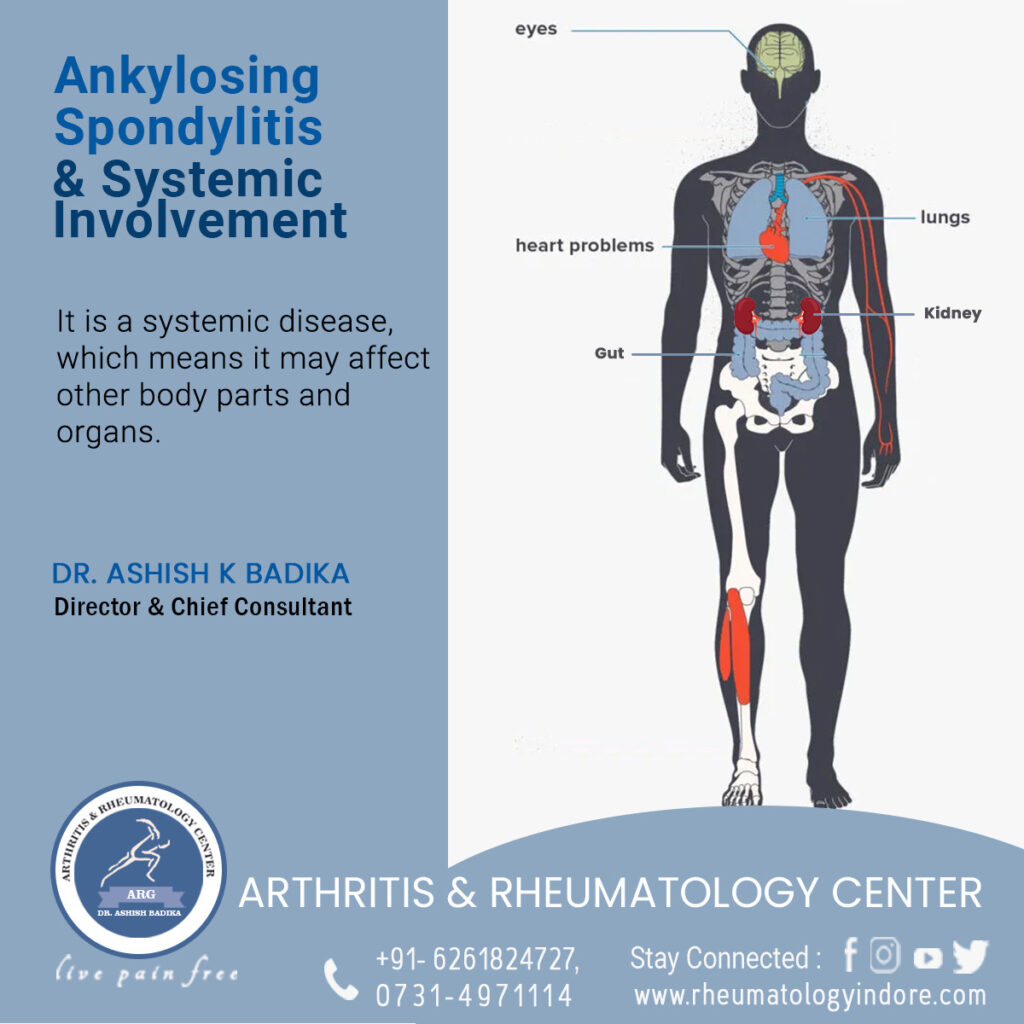
Out of many subtypes of Spondylarthritis most common form is ankylosing spondylitis. Some diseases may have symptoms that closely mimic/resemble Ankylosing spondylitis (AS) and can be mistakenly considered AS.
Few conditions that mimic/ resembles Ankylosing spondylitis:
- Acute back strain or lumbago: – Lumbago refers to lower back pain. The type of lower back pain and the area of pain distribution are the two factors that help in determining the cause of the back pain. In a person’s lower back several anatomical structures can cause extreme back pain and may radiate pain to other parts of the body like the leg.
- Acute or chronic mechanical low back pain: – The patient tends to experience pain in the back and it may last longer. This targets soft tissues, spinal joints, and vertebrae. Some accident or activity you have done might be the reason for the pain.

- Fibromyalgia: -It’s a very common type of condition that might affect muscles and bones. Patients experience symptoms like fatigue, joint pains, and generalized body pains.
- Diffuse Idiopathic Skeletal Hyperostosis (DISH): – DISH leads to the hardening of ligaments particularly in the areas where they are attached to the spine. Common symptoms which might be experienced are stiffness in the upper back, moderate pain. It’s commonly seen in patients with diabetes.
- Sacroiliac joint Infection: – The disease causes inflammation in either one or both sacroiliac joints. It can cause pain in the lower back or buttocks and may radiate pain to the legs.
- Osteitis Condensans ilii (OCI): – OCI is a non-progressive condition. This condition is marked by iliac bone sclerosis and can be found on x-ray/imaging. Symptoms are most commonly seen in case of pregnancy or weight gain. Women are more prone to this disease. It’s is self-limited and its management is conservative.
It is advisable to visit a Rheumatologist to be sure of the disease you are having so that proper treatment can be given.
Dr. Ashish K Badika has 3 years of advanced training in Rheumatology and Clinical Immunology including 2 years Post Doctoral.
He has extensive exposure to Systemic Autoimmune Disorder (Rheumatoid arthritis, Psoriatic arthritis, Seronegative spondyloarthritis, Systemic lupus erythematosus, Scleroderma, Gout, Myositis, Sjogren’s Syndrome, Vasculitic conditions, and Paediatric rheumatology disorders).